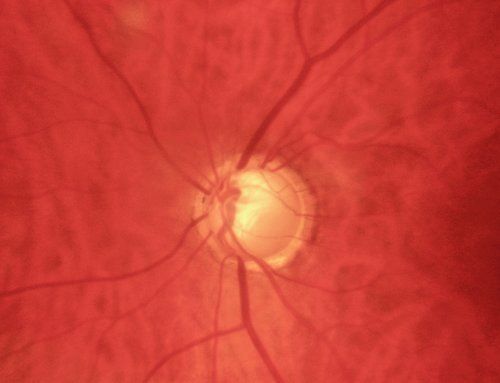
Glaucoma is sometimes known as the “silent blinder” since many people who have it do not know. Symptoms usually do not appear until permanent damage has already occurred. Glaucoma is usually associated with elevated pressure inside the eye (intraocular pressure). When pressure is elevated it can cause damage to the optic nerve which carries images from the eye to the brain. Glaucoma can also develop without an increase in eye pressure, called low-tension or normal-tension glaucoma. Be sure to let your doctor know if you have a family history of glaucoma.
The video above was produced by the American Academy of Opthalmology. Click here for more information.
There are many types of glaucoma with different causes and therefore different treatments. Your eye care provider will determine the best initial treatment for your glaucoma management. Often, these will be eye drops that lower the pressure in your eye. They are several classes of glaucoma drops that work through different mechanisms to lower your eye pressure. Sometimes several drops may be needed to reduce the pressure to a level that is healthy for your eyes. Please see the video below for instructions on how to properly instill eye drops. If the eye drops lose their effectiveness, have too many side effects, or do not lower the pressure enough there are several other treatment options.
The video above was produced by the American Academy of Opthalmology. Click here for more information.
One other treatment option is a laser procedure. One common laser procedures include Selective Laser Trabeculoplasty (SLT). The laser creates spots on the trabecular meshwork that allow for more fluid to escape from the eye which lowers the pressure in the eye. Your doctor will determine if you are a good candidate for this procedure.
Micro invasive Glaucoma Surgery (MIGS)
If you and your doctor have determined you are ready for cataract surgery and you have mild to moderate primary open-angle glaucoma you may be a good candidate for a microinvasive glaucoma surgery (MIGS). This is a procedure that is done at the same time as cataract surgery and increases the outflow of the fluid through a small tube or shunt that is implanted in the trabecular meshwork. This procedure may reduce your dependency on eye drops to lower eye pressure. Your eye care provider will determine if you are a good candidate for this procedure and which device to use.
Click here to learn more about the approved MIGS devices and procedures.
In angle-closure glaucoma, the angle between the iris and cornea is too narrow to allow the fluid in the eye to drain properly. When this happens it can increase the pressure in the eye and cause damage to the optic nerve. To prevent this from happening, a laser will be used to put a small hole in the iris allowing fluid to flow freely from the front to the back of the eye, this procedure is called a peripheral iridotomy.
Rarely in advanced cases of glaucoma a trabeculectomy, filtering bleb, or other types of glaucoma surgery may be needed to adequately control the eye pressure.
Glaucoma Testing
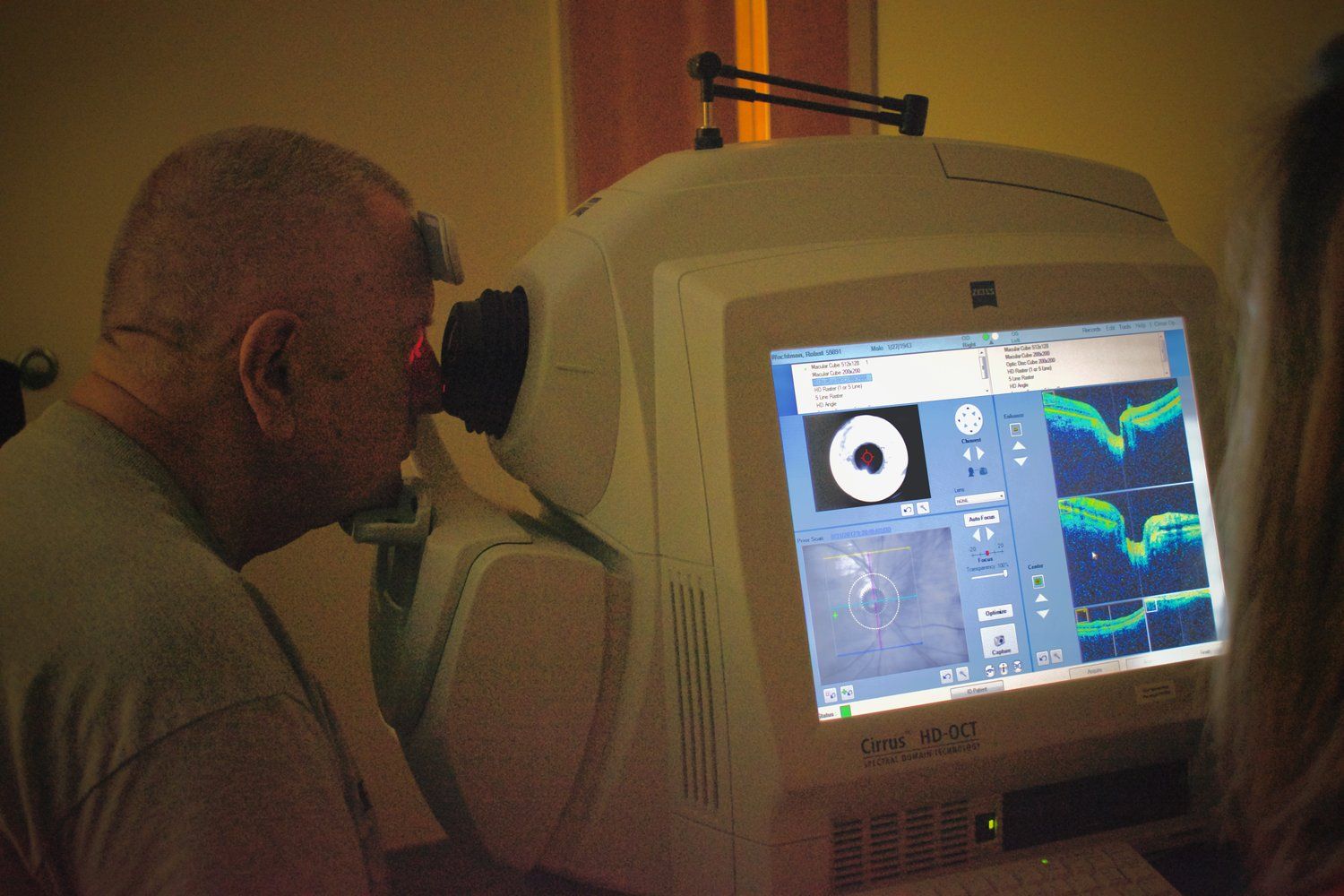
OCT (optical coherence tomography)
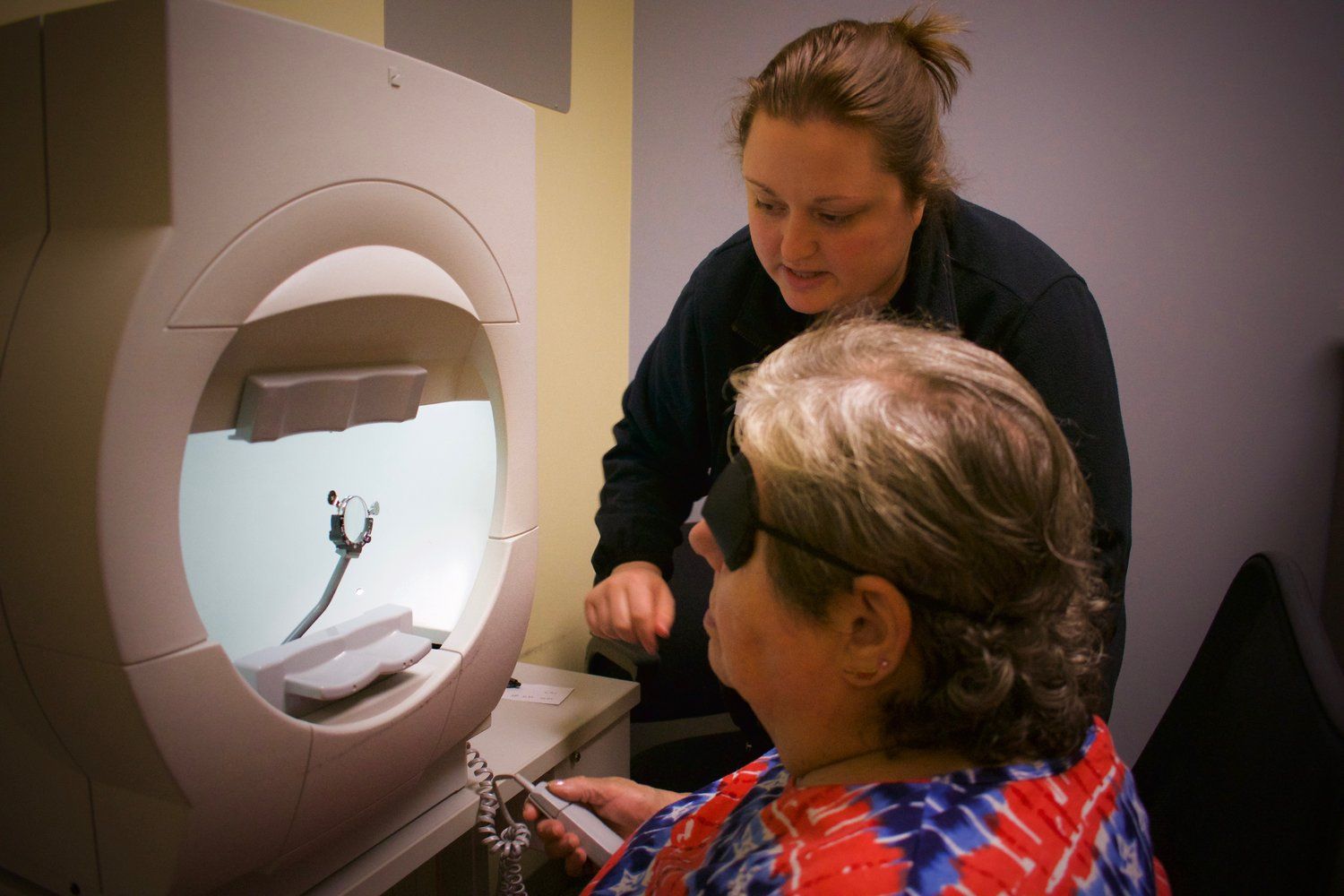
Visual Field

Gonioscopy
Various testing may be done to determine your risk factors for developing glaucoma or if the disease has progressed. One test commonly done is the OCT (optical coherence tomography). This scan allows imaging of the thickness of the retinal nerve fiber layer. Change over time to the thickness of these nerve fibers often indicates glaucomatous damage.
Another test commonly done is a visual field. This is a test of the patient's peripheral vision, which is first affected in glaucoma. The test is performed with one eye at a time and the patient will click a button every time he or she sees a flash of light off to the side.
Gonioscopy is a lens with a mirror that a doctor will rest on the front of the eye like a contact lens. This will allow them to see the angle at which the fluid in your eye drains. This will help determine if the angle is open and the fluid is draining. This is an important test in the diagnosis and management of glaucoma to help determine or rule out some possible causes of glaucoma.
Pachymetry is a measurement of central corneal thickness. This test is used to determine a patient's risk factor for glaucoma, thinner corneas are associated with an increased risk of glaucoma, whereas thicker corneas are oftentimes not as likely to develop glaucoma. However, there can be significant individual variation.
*For additional information regarding Glaucoma, please visit the Glaucoma Research Foundation website here.